GI Bleeding Risk Estimator
Risk Factor Assessment
Estimated Risk Level
Taking a common antidepressant alongside a standard over-the-counter painkiller might seem harmless, but the chemical interaction between them can be dangerous. When you combine SSRIs is a class of Selective Serotonin Reuptake Inhibitors used to treat depression and anxiety with NSAIDs (Nonsteroidal Anti-inflammatory Drugs), your risk of upper gastrointestinal (GI) bleeding jumps significantly. In fact, research shows a consistent 75% increase in bleeding risk when these two are used together compared to using NSAIDs alone. This isn't just a theoretical concern; it's a practical danger for millions of people who manage both mood disorders and chronic pain.
Quick Summary: Key Takeaways
- Combining SSRIs and NSAIDs increases the risk of stomach and intestinal bleeding by about 75%.
- The risk is multiplicative, meaning the combination is far more dangerous than either drug alone.
- Proton Pump Inhibitors (PPIs) can reduce the absolute bleeding risk by roughly 70%.
- Acetaminophen (paracetamol) is a safer alternative for pain relief when taking antidepressants.
- Elderly patients and those with a history of ulcers are at the highest risk.
Why This Combination Is Risky
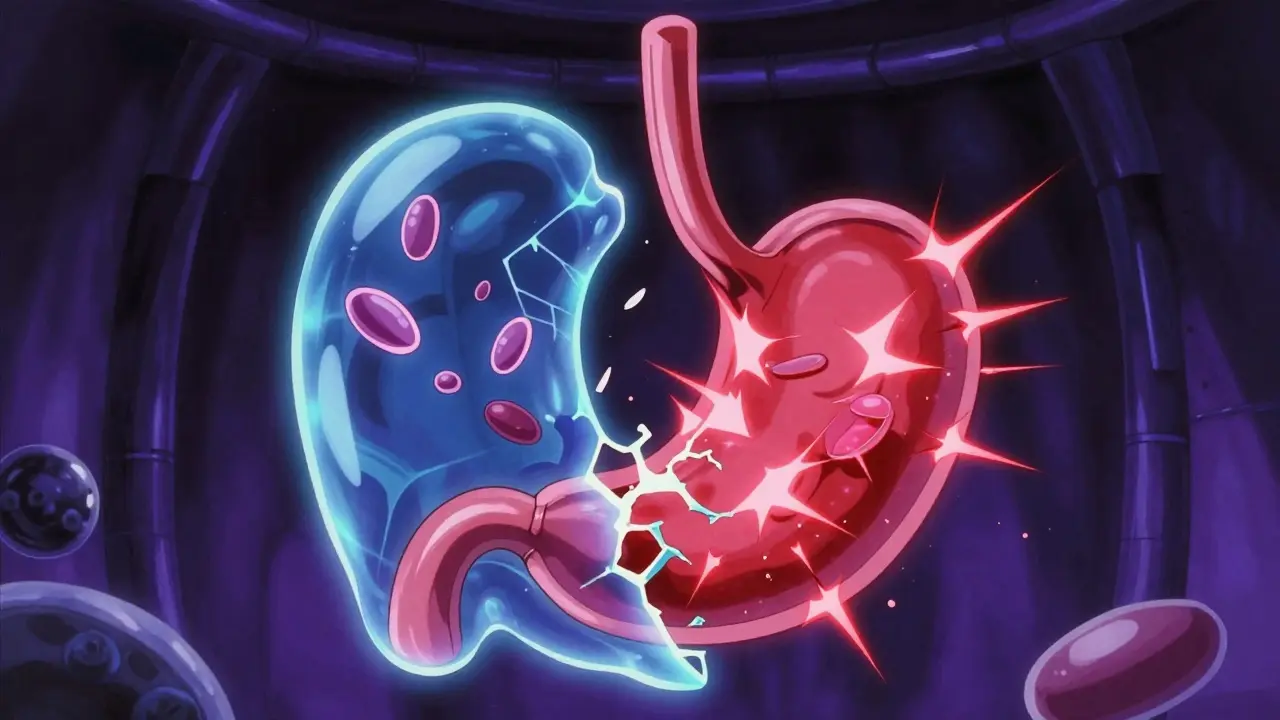
To understand why your stomach is at risk, you have to look at how these drugs affect your blood and your gut lining. Your body uses serotonin not just in the brain, but also in platelets-the tiny cells that help your blood clot. SSRIs block the reuptake of serotonin into these platelets. When platelets can't handle serotonin properly, they can't clump together as effectively to stop a leak. This weakens your primary hemostasis, making it harder for your body to plug a bleeding wound.
At the same time, NSAIDs, such as ibuprofen or naproxen, do two things: they irritate the mucosal lining of the stomach and inhibit the synthesis of prostaglandins. Prostaglandins are essentially the "shield" that protects your stomach wall from its own acid. When you take away the shield with an NSAID and weaken the clotting process with an SSRI, you create a perfect storm for a GI bleed. This dual-pathway attack is why the risk is multiplicative rather than just adding up.
Breaking Down the Numbers: How High Is the Risk?
The data on this interaction is stark. A meta-analysis published in Nature Scientific Reports involving over a million patients confirmed an odds ratio of 1.75 for GI bleeding. For those who also take low-dose aspirin, the situation becomes even more critical. Some studies, including one published in JAMA Internal Medicine, have found that the combination of SSRIs, NSAIDs, and aspirin can increase the risk of upper GI bleeding by more than 12-fold compared to people taking none of these medications.
Not all painkillers are created equal in this scenario. Some drugs are harsher on the stomach than others. For example, COX-2 selective inhibitors are generally safer for the gut than non-selective options.
| Medication Type | Example Drugs | GI Bleeding Risk Level | Mechanism of Risk |
|---|---|---|---|
| Non-selective NSAIDs | Naproxen, Ibuprofen | High | Direct mucosal damage + platelet inhibition |
| COX-2 Inhibitors | Celecoxib | Moderate/Low | Targeted inflammation block, less gut irritation |
| Non-NSAID Analgesics | Acetaminophen | Very Low | No significant effect on platelet function |
Who Is Most at Risk?
While anyone taking this combination should be cautious, certain people are in the "danger zone." If you are over 65, your stomach lining is naturally thinner and your kidneys may process these drugs more slowly, increasing the risk. People with a history of peptic ulcers are also highly susceptible, as the combination can easily reopen old wounds or create new ones.
The duration and dose also matter. The risk tends to climb after 90 days of continuous SSRI use. Similarly, taking high doses of NSAIDs (such as more than 1,200 mg of ibuprofen equivalent per day) significantly pushes the needle toward a potential emergency room visit. Many patients don't realize this until it's too late; reports from patient forums show a high "surprise factor," where people were never warned by their doctors about this specific interaction.
Prevention and Safer Alternatives
The good news is that this risk is manageable. The first and most effective strategy is simple: switch your painkiller. Acetaminophen (known as paracetamol in the UK) does not interact with the serotonin pathways in platelets and doesn't strip the stomach's protective lining. For most mild-to-moderate pain, this is the gold standard for someone on an antidepressant.
If you absolutely must take an NSAID for a condition like severe rheumatoid arthritis, doctors often prescribe a "buffer." Proton Pump Inhibitors (PPIs), such as omeprazole, reduce the amount of acid your stomach produces. By lowering the acidity, PPIs protect the lining and can reduce the absolute bleeding risk by about 70%. This essentially puts a safety net under the patient, preventing small irritations from turning into full-blown hemorrhages.
Practical Steps for Patients and Caregivers
- Audit Your Meds: Check if you are taking both an SSRI (like sertraline or fluoxetine) and an NSAID (like ibuprofen or naproxen).
- Question Your Pain Relief: Ask your doctor if acetaminophen is a safe substitute for your specific needs.
- Request a Risk Assessment: If you are over 65 or have had stomach issues, ask about a PPI to protect your gut.
- Watch for Red Flags: Be alert for "coffee ground" vomit, black or tarry stools, or sudden unexplained fatigue (a sign of anemia from slow bleeding).

The Future of Risk Management
Medical technology is moving toward personalized risk. We are seeing the rise of tools like the GI-BLEED risk calculator, which uses your genetic profile (such as how your liver metabolizes drugs via the CYP2C19 enzyme) to predict exactly how likely you are to bleed. This means in the near future, your doctor won't just guess based on your age; they'll have a percentage-based risk score before they write the prescription.
There is also a shift in the types of antidepressants being used. Some newer options, such as vortioxetine, have shown a lower incidence of bleeding events in clinical trials compared to older SSRIs. As our understanding of the "serotonin-platelet" connection grows, the goal is to move away from the dangerous SSRI-NSAID combination entirely.
Can I take a single dose of ibuprofen while on an SSRI?
A single, occasional dose is unlikely to cause a major bleed for a healthy person, but it still increases the risk. For those with a history of ulcers or the elderly, even a short course can be problematic. It is always safer to use acetaminophen first.
What are the warning signs of a GI bleed?
Look for stools that look black, tarry, or like coffee grounds. Other signs include vomiting blood, severe stomach pain, and symptoms of anemia like extreme dizziness, shortness of breath, or pale skin.
Are all antidepressants risky when mixed with NSAIDs?
The risk is most prominent with SSRIs and SNRIs because they both affect serotonin. Other classes, like bupropion, do not have the same effect on platelets and generally don't carry this specific bleeding risk.
How do PPIs help prevent bleeding?
Proton Pump Inhibitors (PPIs) shut down the pumps in your stomach that produce acid. Since NSAIDs make the stomach wall more vulnerable, having less acid prevents those vulnerabilities from turning into open ulcers that bleed.
Why is the risk higher for elderly patients?
Aging leads to a naturally thinner gastric mucosa and often involves other medications (like aspirin or anticoagulants) that further thin the blood, creating a cumulative effect that makes bleeding much more likely.
Next Steps and Troubleshooting
If you've discovered you are currently taking both an SSRI and an NSAID, do not stop taking your antidepressant abruptly. Doing so can cause withdrawal symptoms or a relapse of depression. Instead, schedule a call with your doctor to discuss a transition plan.
For those managing chronic pain who cannot switch to acetaminophen, ask your provider about a "step-down" approach: try a COX-2 inhibitor like celecoxib first, or implement a daily PPI regimen to mitigate the risk. If you notice any change in your stool color or a sudden drop in energy, seek medical attention immediately, as internal bleeding can be silent until it becomes an emergency.





prince king
April 28, 2026 AT 11:59This is such a helpful breakdown of a really scary topic! It's amazing how much a simple switch in meds can make a difference in our overall well-being 🌟. Just gotta be mindful and listen to our bodies! 😊✨
Amber McCallum
April 28, 2026 AT 20:12People just don't know how to live naturally. Pills for everything and then you're shocked when your body breaks. It's basic karma for ignoring your soul.
Jarrett Jensen
April 30, 2026 AT 12:10While the presented data is ostensibly accurate, the lack of a deep dive into the pharmacokinetic nuances of various SSRI half-lives renders this summary somewhat pedestrian. One would hope for a more rigorous exploration of the CYP450 enzymatic competition rather than these simplified bullet points designed for the masses.
Justin Crice
May 1, 2026 AT 12:33The synergistic effect on primary hemostasis via the depletion of platelet serotonin stores is a fascinating pharmacological intersection. I wonder if the efficacy of COX-2 inhibitors in this context is purely due to the preservation of the gastric mucosal barrier or if there's a more complex interaction with the systemic inflammatory response.
Peter Minto
May 2, 2026 AT 12:53Doctors in this country are a joke!! Probly just want us on more pills like those PPI things. Wake up amerca we dont need these fancy drugs just eat real food and stop complainin about a lil stomach ache!
Angela Cook
May 3, 2026 AT 09:35Exactly! Our healthcare system is a disaster and it's the only thing keeping us from being the strongest nation on earth. Stop importing these Pharma ideas!
Sharon Mathew
May 3, 2026 AT 17:44Oh please! As if a 75% increase is actually some kind of apocalypse! I've taken ibuprofen and sertraline for years and my stomach is absolutely fine. The medical industry just loves to create panic where there is none to sell more "protective" meds like PPIs! Absolute madness!
Timothy Brown
May 5, 2026 AT 11:32Imagine actually believing your personal anecdote outweighs a meta-analysis of a million people. Typical.
Jean Robert
May 7, 2026 AT 10:27I really want everyone to feel empowered here because knowing this information is the first step toward a healthier journey, and if you're feeling overwhelmed by these risks, just remember that you can take small, manageable steps by chatting with your healthcare provider who wants the best for you, and it's totally okay to feel a bit anxious about med changes as long as you move forward with a positive mindset and a little bit of patience for your body to adjust to the safer alternatives like acetaminophen which can be a real lifesaver when handled with care and love for oneself.
Jenna Riordan
May 8, 2026 AT 19:52I bet some of you reading this are terrified now. Maybe you should check your medicine cabinets right now and tell me exactly what you're taking so we can see who's actually in danger.
Raymond Lipanog
May 9, 2026 AT 19:25It is prudent to maintain a balance between clinical caution and the practical necessities of pain management. While the pharmacological risks are evident, one must consider the holistic impact on a patient's quality of life, ensuring that the prevention of a potential bleed does not inadvertently lead to unmanaged chronic suffering.